We have several significant Talking Mats changes this month – in our Website, our Shop and the Digital Talking Mat
Shop:
Visit our new shop for information about our full range of products. There is now have a much improved journey to make it easier for customers wanting to buy training and resources. http://www.talkingmats.com/shop/
Digital Talking Mats:
Following a process of integrating feedback from our customers Phase 2 of the Digital Talking Mat (DTM) is now complete. The features include:
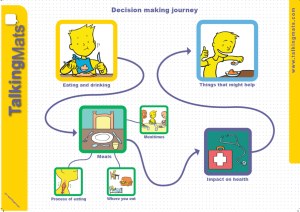
- Easy access to a wide range of symbol sets relating to health and well-being, structured in thematic groups. The design means you cannot lose or mix the symbols up.
- An intuitive design which automatically prompts the user through the Talking Mat framework
- An ability to import relevant photos or images from your camera role or web to personalise the mats or create sub-mats.
- A secure log on to protect confidentiality
- Storage of previous mats on the internal DTM filing system allows reflection and progress evaluation
- Facility to email completed mat, additional comments and action plan directly to relevant team members.
Our customers have told us that a subscription model is challenging for organisations to manage so we have shifted to a one off purchase. We understand that organisations will require their staff to have more than one log on and we have a scheme to allow you to do that at a significantly reduced cost. Click here to see how multiple digital logons can be bought DTM Organisational Logon
Customers using the DTM are excited by its easy to use design and time efficient solution to person centred intervention.
To see the Digital Talking Mats in Action click here
If you would like to read more please follow the links to some of our blogs:
Using the app to develop EHC plans
http://www.talkingmats.com/ehc-plans-with-the-talking-mats-app/
Adding photos to personalise the mats
http://www.talkingmats.com/adding-photos-to-your-digital-talking-mat/
eHealth Good Practice Case Study
http://www.ehealth.nhs.scot/case-studies/talking-mats-nhs-forth-valley/?platform=hootsuite
We are very grateful to Anna Volkmer for sending us this blog, Lets Talk about Capacity…
She has just had an excellent book published – Dealing with Capacity and Other Legal Issues with Adults with Acquired Neurological Conditions http://www.jr-press.co.uk/dealing-capacity-legal-issues.html. In it she describes how AAC methods, including Talking Mats, can be used to support people in expressing their decisions.
Prior to 1959 people who were considered “non-compus mentis” were cared for under the “parens patriae” principle. Literally translated this meant that they were ‘parents of the country’ and decisions to protect them and their property were made by the Crown (the Lord Chancellor). These people were often described as “Chancery Lunatics”. In 1959 the “parens patriae” jurisdiction gave way to the Mental Health Act. This Act instructed that “the judge may, with respect to the property and affairs of a patient, do or secure the doing of all such things as appear necessary or expedient…for making provision for other persons or purposes for whom or which the patient might be expected to provide were he not mentally disordered” (section 102 (1)(c)). Unfortunately, this Act did not make adequate provision for non-financial decisions such as medical decisions. During this period it was case law that guided professionals in supporting their patients who lacked capacity in medical decision making. It was not until 2005 that the first Mental Capacity Act was given Royal Assent, accompanied by the Mental Capacity Act Code of Practice in 2007.
I returned to the UK from a 5-year stint working in Melbourne, Australia, just after the Mental Capacity Act had been published. Mental capacity was on the tip of everyone’s tongues and as the speech and language therapist working on a multi-disciplinary team I became an integral part of this process. Patients I was seeing, often people with primary progressive aphasia or other types of dementia, were asking about how to make future decisions. They and their families were keen to understand how the mental capacity act worked, how to prepare for the future and how to have their voices heard. On the other side of the coin I was working on an inpatient ward where staff were concerned about ensuring we were fully assessing the decision making capacity of people with cognitive and communication difficulties, often holding best interest discussion to plan for the future of these individuals. Many of these decisions related to dysphagia, but others related to accommodation and finances.
What concerned me was the lack of evidence available across the speech and language therapy arena in this area. There was little to none in terms of written research, let alone written advice or even examples of good practice tailored to speech and language therapy clinicians. As I asked around I found an enormous disparity in the services that speech and language therapy clinicians were providing across different trusts. I had previously written a book on dementia, and had included a chapter on assessments of decision-making. At this stage some of the only research related to communication and decision-making had come from Talking Mats. This had demonstrated that using the talking mats tools can support families and caregivers in conversations with their loved ones when discussing decisions to be made. They found that conversation enabled people in understanding, retaining and expressing themselves in decision-making discussions.
Following a particular stimulating discussion with the publishers at J&R press, they invited me to submit a book proposal on this topic. As I was developing this idea I found the topic of mental capacity was raised more and more often at study days and seminars I attended. At these study days I started linking in with more like minded speech and language therapists such as Mark Jayes, Hannah Luff and Claire Devereux. These were clinicians who all agreed on the diversity of our potential role in supporting our patients around mental capacity issues. These common interests enabled a collaboration. Our book is now published.
Through these connections I became aware of other work being done; Mark Jayes holds a NIHR doctoral fellowship award and is conducting research in the development of a communication and capacity assessment tool kit. Claire Devereux is the chair of the Southern Psychiatry of Old Age Clinical Excellence Network, together we have held a workshop with the clinical specialists where we developed a consensus document on role of the speech and language therapist in capacity assessment. This is to be published in Bulletin magazine later this year. Hannah Luff is a clinical lead speech and language therapist at South London and the Maudsley NHS Trust and is currently a member of the review panel looking at the NICE SCIE dementia guidelines.
The wonders and value of networking never ceases to delight, enthuse and inspire me! And you can purchase our book at the following website (there is currently a discount rate until 21st February):
http://www.jr-press.co.uk/dealing-capacity-legal-issues.html
You can follow me on my blog https://annavolkmersbigphdadventure.wordpress.com/ or on twitter @volkmer_anna
Following the success of previous seminars we are holding further specialist seminars in Stirling and London for anyone who has done the Talking Mats training. The topics will be:
- Talking Mats and the Eating and Drinking resource (morning)
- Talking Mats and Capacity (afternoon)
During the Eating and Drinking seminar, we provide background on how and why the resource was developed and showed some DVD examples of people using the resource. This really brings things to life and shows how important it is to give people (with and without speech) the opportunity to consider and talk about different aspects of eating and drinking. We also give people hands-on practice in using the symbols from each topic. Each participant will receive a copy of the full Eating and Drinking resource, including symbols, a mat, and explanatory booklet.
During the Capacity seminar we will discuss the fundamental principles of the Capacity Act and participants will have a chance to consider how Talking Mats can help people to:
- understand
- retain/remember
- weigh up information
- communicate their views/wishes and feelings.
They will also be given the opportunity to work through some practical examples and think about options to help people understand issues and make decisions.
If you have completed a Talking Mats training course and would like to attend either of specialist seminars, please click on the relevant course and fill in the registration form.
Stirling on Friday 29th April Stirling Seminars flier Apr 2016
London on Friday 10th June London Seminars flier June 2016
Registration form Seminar registration form 2016
Do you want a part time, time limited opportunity to work for Talking Mats based in the North West of England? We are appointing an External Associate to extend access to resources and training in this part of the country. We would like this person to
- generate interest and business in the North West of England in Talking Mats with a focus on children and young people, particularly the promotion of the use of Talking Mats in the SEND(Special Educational Needs and Disability) reforms
- work with Talking Mats to promote a marketing seminar in the North West
- work with Talking Mats to run training and establish a base for a North West training programme
- increase sales in Talking Mats in the North West of England
If you have extensive experience of using Talking Mats to allow children and young person to have a voice particularly in their education, health and care plans and are passionate about extending the reach of this framework to a range of services then please consider whether this opportunity maybe right for you. We are looking for someone with initiative ,enthusiasm for the role of Talking Mats, good local professional networks and great communication and networking skills.
Please down load the person spec, project role and how to apply here Talking Mats External Associate
Closing date is the 28th Feb with interview scheduled for the 7th March .if you want to discuss further then please phone the Talking Mats office and ask to speak with either Lois or Margo.
This is the second of Kristine Pedersen’s projects using Talking Mats as a tool to support people with dementia.
Care workers at two residential care homes in Denmark were taught how to use the Talking Mats framework and how to incorporate the method into planning daily activities for people with dementia.
The care workers gave positive feedback in regard to using Talking Mats:
- Using the Talking Mat framework provides important knowledge about communicative difficulties of the person with dementia
- Talking Mats helps people to understand their options and thereby motivates to social activities, eating, physical exercise, etc.
- Talking Mats increases the possibility of active participation in caregiving plans
- Talking Mats enhances the joy of work, when I know how I can give the right care
- The Talking Mats conversations support a closer relation between elderly and care giver
This project and the one described in the previous blog, gave the opportunity to explore the Talking Mat framework in use and how the framework can support the communication of people with dementia. Very importantly, due to the adoption of Talking Mats and its extension in Denmark, the projects gave a lot of Danish examples. The projects also gave important information about how to implement the tool in care homes for people with dementia within a Danish setting.
‘We are very grateful to the Directors, Dr Joan Murphy and Lois Cameron and everyone on the team at the Talking Mats Centre who developed the framework and who continue to increase knowledge of Talking Mats through research and education. It is a very helpful tool for many people and supports and enables more people to have their views seen and heard’
And we are grateful to Kristine for sharing her projects with us.
 Online training login
Online training login