Talking Mats have been part of an exciting research project which looked at whether the Digital Talking Mat App could improve health and housing outcomes for social housing tenants.
Working together with tenants and staff from Loretto Housing and Care, Stirling University, Napier University and Age Scotland we have developed and piloted a new Talking Health and Housing set for the Talking Mats App!
Project Aims
The aim of the project was to:
- Develop an App that would support social housing tenants with communication difficulties to say what they thought about their Housing and Health.
- To improve communication between social housing tenants and health professionals.
Researchers were also keen to see whether the App would help to demonstrate the link between tenants’ housing and health solutions.
What we did
The Talking mats team facilitated two focus group sessions with all the partners to decide what topics were needed.
Once the mats had been completed the researchers from Stirling University and Napier University conducted interviews and focus groups with staff from Loretto and related Health professionals and then analysed the data from the mats.
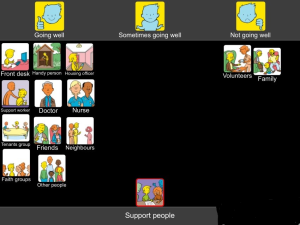
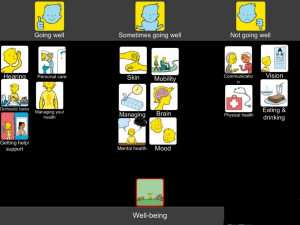
The Talking Health and Housing set
The set has three topics: Home, Wellbeing, Support people
The Top scale for this set is Going well…Going well sometimes…Not going well
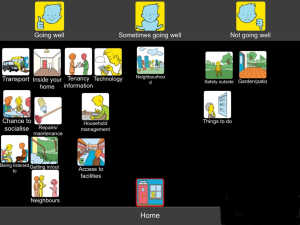 One of the major themes to emerge was safety inside and outside the house. Using the App, tenants were able to identify issues that were making them feel unsafe including:
One of the major themes to emerge was safety inside and outside the house. Using the App, tenants were able to identify issues that were making them feel unsafe including:
- A broken stair door
- Uneven pavement outside the house,
- Poor eyesight
- Poor mobility
This was having a negative impact on tenants’ wellbeing and by doing the mats, actions were identified to address all these concerns and anxieties were reduced.
It was a great partnership and we hope to work together again to further explore how the App can support the Service Integration agenda by facilitating communication between Health, Social and Care and Housing with the tenant at the centre.
Read the summary report 201908 Talking Health and Housing Summary Report
If you are interested in finding out more about the Talking Health and Housing App please email info@talkingmats.com
The Symbols are designed and © to Adam Murphy 2015 and assigned to Talking Mats Ltd. in perpetuity. They may not be reproduced without permission
Many thanks to Marit Boot, founder of the charity What? Why? Children in Hospital for this guest blog sharing information about the fantastic family-friendly videos they make to help children understand hospital procedures.
As a mum, I know the worry when your child is ill and needs tests in hospital. It’s the not knowing what is wrong, understanding all the different tests and how to explain them to your child. That’s why I founded the What? Why? Children in Hospital charity to make family-friendly videos about hospital. So when we make a new video explaining a procedure in an easy to understand way, it’s the reaction from parents that makes it worthwhile. The relief, that they now have an idea of what will happen and that they can share the video with their child, it makes their preparation much easier. I want to share with you the story of one of the mums in our latest video. Louise talked to us about Rocco’s gastrostomy feeding tube operation.
“We didn’t have anything like the videos WWCIH make when Rocco first had the gastrostomy surgery. Being a parent in that position is daunting. You want to do what’s right for your child but there’s so much to take in. It isn’t always easy to remember what you’re told in the doctor’s office. So when we had the opportunity to help other worried parents and children by making this video, we jumped at it.”
Thousands of children go through a gastrostomy procedure in Scotland every year. It’s a major procedure and can be a complex idea to communicate to children and anxious parents. In the videos, medical specialists talk through how a gastrostomy feeding tube works, how the procedure is done and how parents should look after the feeding tube at home.
The videos are absolutely fantastic! With 32 doctors, nurses and specialists helping to deal with my son’s complex needs, it can be overwhelming to take in information they give to us. These videos are amazing for parents to find out information when they’re ready to absorb it. Even if that’s when you finally get to sit down at 2am.Gastrostomy is major surgery and we had to weigh the risks against the benefits for Rocco’s life. There was so much to take in, about the operation, the aftercare. At one point the doctor used a teddy to show how the tube worked – it was useful but didn’t give the full picture. The videos What? Why? have made cover what you need to know in a calm, thoughtful way. They will be a huge help to worried parents and will help them explain to their child what will happen and why. They should make as many videos as possible!”
We have 55 videos on our YouTube channel about tests such as MRI, CT, ECG, ultrasounds, allergy tests, breathing tests and sleep studies and we are always making new ones. They’re made in partnership with children’s hospitals in Scotland and are suitable for school-aged children, children with learning difficulties and autism as well as parents and carers from all cultural backgrounds and literacy levels. The videos have already been viewed by 2.8 million families across the world.
If you know a parent or carer who’s worried about their child going to hospital send them to our YouTube page (WWCIH charity), Facebook page (@wwcih) or our website: www.wwcih.org.uk
And if there’s a procedure you think we should look at next, get in touch! We’re here to help children and parents just like you!
info@wwcih.org.uk
Marit Boot, Founder What? Why? Children in Hospital, July 2019
What an amazing day we had celebrating 21 years since the first article about Talking Mats was published in August 1998 in the Communication Matters journal. Over 180 people attended from so many different walks of life. We are grateful to them all for coming and helping us mark the occasion. We are also grateful to the endowment fund of Forth Valley NHS for helping us fund the event.
In the morning thanks to a fantastic group of speakers we discussed a diverse range of topics:
- Rachel Woolcomb, our OT associate explored how she sees Talking Mats as an ‘energy efficient’ thinking tool and outlined how it supports people to think through issues Talking Mats as a Thinking Tool

- Two teachers, Fiona Graham and Claire Forgan examined the benefits and challenges of embedding Talking Mats in school to encourage and extend pupil participation
- Susan Gowland, a speech and language therapist discussed the use of Talking Mats in a forensic setting illustrating from a case example how Talking Mats helped staff see that incidents do not come out of the blue. When they looked at the pattern of mats over time they could see when the patient was expressing concern about small things. This was an indication that bigger things were going on for him.
- Sally Boa the Research Manager for Strathcarron Hospice led on how Talking Mats was a way to enable ‘end of life’ conversations, things that can be hard for any of us to talk about. The mats give a safe space and structure to enable these conversations to take place. Talking Mats and Palliative care
- Two parents Tracey Campbell and Sarah Robertson spoke about their experience with using Talking Mats with their children. Sarah said ‘Talking Mats gives us a happier home. It helps me be patient, listen and give power to him’ (her son). Talking Mat A Parents View 15.08.19
- Jill Bradshaw of the Tizard Centre, University of Kent outlined her research including her work exploring Talking Mats as a tool to sit beside functional analysis of behaviour where the person’s own view of what challenges and helps them is often overlooked and not included fully. TM and PBS final version for handout
- Anne Lafferty of The Advocacy Project , give a powerful example of using Talking Mats in a legal setting. This important work is in need of funding so we can explore this more fully. Everyone also got to play legislation bingo! Talking Mats and Supported Decision Making PP 2
- Liz Taylor (Talking Mats licensed trainer) and Lynnette Linton (Talking mats co-trainer) from The Action Group shared their experience in a fantastic film. They used a Talking Mat to reflect on the experience and would recommend co-training as an effective way to deliver the Foundation course.
- Brian Robertson and Paddy Carstairs described how they developed a Talking Mats to allow members of the National Involvement Network to explore with other people with a learning disability how The Charter for Involvement related to their life experience.This is an empowering way of using Talking Mats that shows that people who get support can help change and improve the support of other supported people.This is an empowering way of using Talking Mats that shows that people who get support can help change and improve the support of other supported people.
- Rosie Noyce from Pennine Care NHS described a whole team approach to supporting Healthy Young Minds and how they have embedded Talking Mats into their care pathway. She cited powerful case examples of impact and a real commitment by the team to hear the voices of young people Talking Mats and Young People’s Mental Health
And that was just the morning! Lots of delegates have asked for copies of the presentations so watch this space
The afternoon demonstrated just how far Talking Mats has come through its partnerships with other organisations. We are so grateful to all the people who came and had stalls and engaged with our networking activities! There was a real buzz in the room as people explored the variety of ways in which Talking Mats is used to support and enable more effective communication. Lots of connections were being made, people thinking about new ways of working and applying Talking Mats in their settings. People enjoyed seeing old friends but was good to see new networks were being built.
So, thank you Care Opinion, Turning Point Scotland, The Action Group, Capability Scotland, The CALL Centre, The Indigo Group, The National Involvement Network, Forth Valley NHS, The Stirling University Careers Service and Alzheimer Scotland. In addition, Talking Mats had a stand with all its products. Also, to promote our Birthday offer since we are 21, we have a 2 for 1 offer on resources for 21 days so order quickly. It ends on the 5th of September!
Today was also the day that Joan marked her ‘retirement’.  She gave a very moving speech that celebrated her distinguished career and her very significant achievements. She leaves an amazing legacy in the Talking Mats framework and with all the energy in the room we are sure it will continue to grow and develop. Thank you, Joan.
She gave a very moving speech that celebrated her distinguished career and her very significant achievements. She leaves an amazing legacy in the Talking Mats framework and with all the energy in the room we are sure it will continue to grow and develop. Thank you, Joan.
Talking Mats is now used in many countries all over the world. As part of our #TMis21 blog series, we wanted to share this great example of Talking Mats being used in Germany.
In March 2019 Prof. Dr. Norina Lauer (OTH Regensburg) and Elena Maxheimer held a lecture and a workshop about Talking Mats at the “aphasia days” in Wuerzburg, Germany. Many thanks to Norina and Elena for sharing information about the “aphasia days” for this blog post.
The “aphasia days” are a large congress – unique in Europe – for people with aphasia, family members and speech and language therapists (SLT). Every year around 600 people from Germany, Austria, Switzerland and Hungary are coming to this event. There are talks, workshops and podium discussions held by participants with aphasia, family members or SLTs. In front of approx. 150 listeners Norina and Elena gave a lecture about Talking Mats and the results of Elena’s bachelor thesis, in which she worked with people with aphasia, who learned to use Talking Mats.
In a three-hour workshop at the “aphasia-days” Norina and Elena taught nine people with moderate to severe aphasia how to use Talking Mats. All persons brought their own tablets and logged into their own account. They where shown how to choose a topic and a top scale and practiced in teams of two. All of them conducted several sessions with different topics and switched partners a couple of times. They had a lot of fun talking about things that matter to them and learn more about their peers. At the end of the workshop they were able to use Talking Mats themselves and are going to use it with their relatives and friends at home. As the workshop was very well received by the participants, it is likely to be repeated at the next “aphasia days” 2020.
If you would like to find out more information about Talking Mats in Germany, and the Digital Talking Mats app which is now available in German, check out https://www.talkingmats.com/talking-mats-in-germany/ and https://www.talkingmats.com/german-digital-talking-mats-with-people-with-aphasia/
Our Talking Mats is 21 Event is in Stirling on Thursday 15th August 2019. Thanks to funding from NHS Forth Valley endowment committee the event is free but you do need to book your space https://www.eventbrite.co.uk/e/talking-mats-is-21-tickets-62362171935
You can come to the morning only, afternoon only or come for the whole day.
If you can’t come to our event watch out for out blogs and social media celebrating the reach of Talking Mats for 21 days before the 15th of August. Please join in with your contributions using the hashtag #TMis21. For 21 days after our event we will be having a special Birthday offer! Watch this space, more to follow …….
Rachel Woolcomb, our Talking Mats OT Associate, shares a recent personal experience where she used Talking Mats to support a difficult conversation:
The vision of Talking Mats is to improve the lives of people with communications difficulties. I have been reflecting recently on the definition of ‘communication difficulties.’
When I first heard about, and started to use Talking Mats 10 years ago, my perception was that it was fantastic for those that could not speak but I must admit I didn’t really consider using it with people who, such as myself, could use their voice to communicate.
Over the years as my understanding has developed, and I have looked further into the use of Talking Mats as a ‘thinking tool’ I have come to a different conclusion.
I would like to suggest that at some points in our lives, each one of us is likely to experience a communication difficulty. I don’t mean that we cannot physically speak, but that we cannot express what we really want to say in words. Perhaps a topic is too difficult to talk about with someone so we don’t bother, or we are overwhelmed by the subject that we don’t really know where to start.
One such subject is that of death and dying.
We know it will happen to us all one day but to talk openly with loved ones, is for some reason, too much to comprehend, too emotive, or considered bleak.
I am very fortunate enough to have grandparents in their 90’s however the conversation about their wishes for the future goes unspoken. It is a challenge for my parents to raise the issue therefore it remains the big unknown.
This is a common problem. In 2009, The National Council for Palliative Care wanted to address this issue and set up the Dying Matters Coalition in England and Wales, to help people talk more openly about dying, death and bereavement and to make plans for the end of life.
Talking Mats have produced a set of topic cards called ‘Thinking Ahead.’ https://www.talkingmats.com/product/thinking-ahead/
These were created in consultation with Strathcarron hospice to help people with advanced illness or long term conditions to think ahead and plan for the future. The three topics in the set are: Affairs, Care and Treatment and Personal Values.
My Mum was interested in my role with Talking Mats and wanted to understand what it was all about. We had already started to talk about the challenges of having difficult conversations, especially about death, and therefore over a drink, in a relaxed coffee shop, we embarked on a journey of discovery using a Talking Mat. My Mum as the Thinker and myself as the Listener .
She used the Talking Mat to help her think about things she had not considered and was able to make plans about what she wanted to do next. I heard her wishes and her thoughts, on why certain things were important to her. It was a very special time, facilitated by a Talking Mat.
My challenge to you as readers of this blog is to ask yourself ‘what do I have difficulty talking about’ – A Talking Mat just might be the answer!
Another resource you might find helpful is ‘Let’s Talk about Death and Dying’ – www.ageuk.org.uk
Rachel will be running a ‘Talking Mats as a Thinking Tool’ workshop at our Talking Mats is 21 Event is in Stirling on Thursday 15th August 2019. Dr Sally Boa from Strathcarron Hospice will also be running a ‘Talking Mats in End of Life Care’ workshop at this event. Thanks to funding from NHS Forth Valley endowment committee the event is free but you do need to book your space https://www.eventbrite.co.uk/e/talking-mats-is-21-tickets-62362171935
You can come to the morning only, afternoon only or come for the whole day.
If you can’t come to our event watch out for out blogs and social media celebrating the reach of Talking Mats for 21 days before the 15th of August. Please join in with your contributions using the hashtag #TMis21. For 21 days after our event we will be having a special Birthday offer! Watch this space, more to follow …….
At Talking Mats, we offer a range of training models https://www.talkingmats.com/training/ that are tailored to suit individual teams and/or organisations and that help them develop their services to people with communication disability.
The one which best supports participants to embed Talking Mats in their practice /organisation is the Enhanced Talking Mats training https://www.talkingmats.com/training/bespoke-training-for-organisations/. This course is run over 2 days with the second day usually 4 months later supporting staff reflect, refresh and extend the implementation of Talking Mats with their clients. It includes an evaluation of the participants’ views of their interaction with ‘thinkers’ before and after the Talking Mats training. Participants are asked to complete a short questionnaire designed by the Talking Mats team on Survey Monkey prior to the first training day.
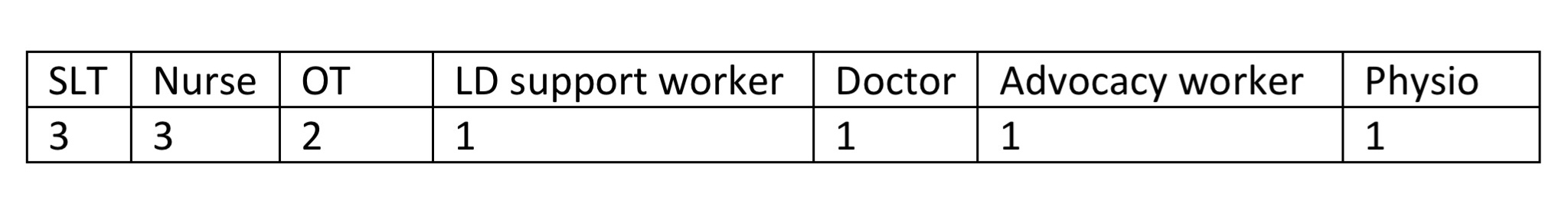
In November 2018 Joan Murphy ran the first day of an enhanced course in Welshpool, North Powys for 12 NHS staff including (Click to enlarge):
Over the next few months participants were asked to use Talking Mats and bring case studies to the follow up day. They were also asked to complete the survey before the second day which was held in March 2019.
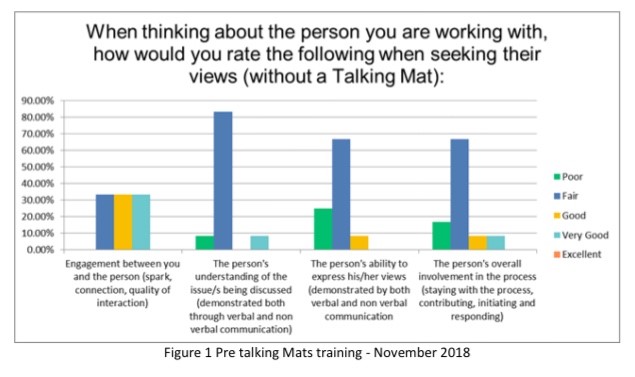
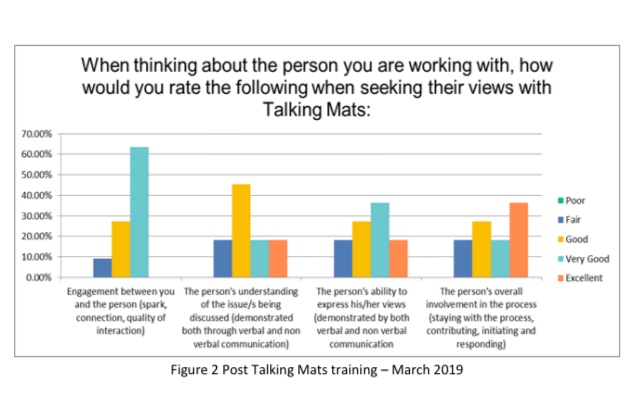
The following graphs show the comparison of the pre- and post- training evaluations. (Double click to enlarge the figures):
Figure 1 Pre talking Mats training – November 2018
Figure 2 Post Talking Mats training – March 2019
In addition, participants were asked to add any comments. Here are a sample of them:
It allowed me to identify areas that mattered most to the person in terms of what they wanted to work on in therapy. It showed me that what I thought was the most severe aspect wasn’t always what was having the biggest impact.
- Now have understanding of hobbies/likes to interact with on the ward to engage in therapy and reduce anxiety/boredom.
- Brought up something important to them which probably would not have surfaced without TM.
- Used to make patient-centred goals as opposed to goals set with family therapist.
In conclusion, if any organisations are looking for Talking Mats training, we would encourage them to consider booking the enhanced course to support them to use Talking Mats to its best effect.
Our Talking Mats is 21 Event is in Stirling on Thursday 15th August 2019. Thanks to funding from NHS Forth Valley endowment committee the event is free but you do need to book your space https://www.eventbrite.co.uk/e/talking-mats-is-21-tickets-62362171935
You can come to the morning only, afternoon only or come for the whole day.
If you can’t come to our event watch out for out blogs and social media celebrating the reach of Talking Mats for 21 days before the 15th of August. Please join in with your contributions using the hashtag #TMis21. For 21 days after our event we will be having a special Birthday offer! Watch this space, more to follow …….
Last week, Laura Holmes, our NW England Associate, had the pleasure of interviewing our inspirational Founder, Joan Murphy. Joan will be retiring after our Talking Mats 21 event on 15th August 2019 and so this was a great opportunity to find out more about her Talking Mats experiences:
Are there any stand-out moments for you, from your Talking Mats time?
Talking Mats are now used in many countries across the world and it has been great to have the chance to travel widely. One particular moment which stands out for me was during one of two trips I made to China with Sally Boa. I was asked to demonstrate Talking Mats with a man who was in hospital having had a stroke. He had no speech and was using a wheelchair. I used Talking Mats to find out what the man felt he could/ couldn’t do. The man shared that he felt he could walk. I had to present the symbol three times as the family members and medical staff watching were adamant that the man could not walk. On the third time, the man pushed the table, moved his wheelchair back then stood up and walked around the room. His family and medical team were completely shocked and realised that no-one had actually thought to ask him if he could walk. This was a massive turning point both for the man – and also for his family and medical team, who could now see the power of using a Talking Mat.
Have you done any Talking Mats yourself that helped you to make an important decision for you or your family?
Absolutely – quite a few! My husband and I both used Talking Mats for our Power of Attorneys and shared them with our lawyer and grown-up children. My husband and I also used Talking Mats to talk about the Scottish Referendum as we had opposing views – it really helped as it made us listen to each other without interrupting. We then went on to use the mats as part of a presentation. Various members of my family have used mats to explore personal issues and decisions
What are the top tips you have gained from your Talking Mats journey – from working in the NHS and then more recently as a social enterprise?
You have to have humour. And be able to listen. It has been essential to be able to work in partnership with Lois and the other Talking Mats team members. The team are such nice people to work with and we have lots of laughs. Setting up as social enterprise was vital for Talking Mats – in terms of having the freedom to be creative. It felt as though someone had a big rubber band which was able to be released. It was a huge risk and there have been lots of leaps of faith along the way.
Do you have any top tips for people using Talking Mats in the Listener role?
Be quiet – and Listen! It’s also important to feel relaxed and to have a sense of humour whilst using it. A Talking Mat is not a test – it is serious, and can be used to explore difficult issues, but it should be fun.
Talking Mats is a low-tech AAC system – do you think it has a place in the modern world?
It is absolutely crucial! Low-tech resources are fundamental in terms of being able to have and develop conversation skills and social closeness.
What do you want for Talking Mats in the next 10 years?
World Domination! Talking Mats has the potential to be used everywhere in the world, by everyone. However I would like to see Talking Mats continue to have a small core team, but increasing Licensed Trainers across both the UK and the rest of the world.
Our Talking Mats is 21 Event is in Stirling on Thursday 15th August 2019. Thanks to funding from NHS Forth Valley endowment committee the event is free but you do need to book your space https://www.eventbrite.co.uk/e/talking-mats-is-21-tickets-62362171935
You can come to the morning only, afternoon only or come for the whole day.
If you can’t come to our event watch out for out blogs and social media celebrating the reach of Talking Mats for 21 days before the 15th of August. Please join in with your contributions using the hashtag #TMis21. For 21 days after our event we will be having a special Birthday offer! Watch this space, more to follow …….
Many thanks to Jenny Trott for our new guest blog about her interview with Talking Mats Director, Lois Cameron – Jenny’s video provides some great information about the Talking Mats approach and our original and digital resources:
A year ago I started my YouTube channel (www.youtube.com/jennytrott) as a way of supporting parents and carers with information and inspiration. As a parent of a disabled child myself I knew that one of the best ways to find out things is from other parents, and YouTube was just a different and new way to do that. To date I have published nearly 50 films about subjects ranging from Self Directed Support to Rebound therapy, and including interviews with parents, professionals and disabled people.
Quite early on I knew that I wanted to make a film about Talking Mats. I had used Talking Mats when I worked with people living with dementia, and I knew that my son’s school were using them too. I had seen the benefits of this innovative communication tool but I also knew that many parents and carers didn’t really understand it because they hadn’t been given the right information.
Lois was kind enough to agree to join me in front of the camera, so in April I visited Talking Mats in Stirling with my tripods, microphones and cameras. It can be a bit daunting interviewing someone I’ve not met before but Lois instantly put me at ease and had the great idea of demonstrating a Mat rather than just talking about it. It was so interesting, experiencing using a Mat first hand and it helped to show the viewers what Talking Mats is really about.
You can view the video here: https://youtu.be/Fmyt1fE-_U8
The feedback from the film has been great, both from professionals, parent carers and SLT students; lots of lightbulb moments; “ah, now I get it”!
I am still making films but less frequently as I am now also setting up a social enterprise, Mecoco (www.mecoco.org) here in North Ayrshire. We’ll be offering work experience and volunteering opportunities to disabled people to work alongside us making candles and melts. I am sure Talking Mats will be invaluable in our workshop!
If you’d like to find out more about accessing Talking Mats training take a look here- https://www.talkingmats.com/training/ – we offer a range of options including online, and bespoke training for organisations, as well as advanced courses and specialist seminars for those who have already accessed Talking Mats Foundation Training.
We are all looking forward to celebrating Talking Mats is 21 on the 15th August
The morning is aimed at people who are experienced Talking Mats practitioners and will extend thinking and Talking Mats practice. There are an interesting range of parallel sessions to choose from. Each participant will get to choose three topics to attend.
- Talking Mats as a Thinking Tool
- Embedding Talking Mats in Schools
- Talking Mats in Forensic Settings
- Talking Mats in End of Life Care
- My experience of using Talking Mats as a parent
- Talking Mats and Positive behaviour Support
- Talking Mats and Supported Decision- Making
- Empowering people with Learning Disabilities to be Talking Mats Listeners and Trainers
- Talking Mats and Children’s Mental Health
The afternoon is more informal and there will be an opportunity to engage with some of our partners – see how they use Talking Mats and try things out . There will be posters on the use of Talking Mats in lots of different places and for a wide range of applications.
Plus there will be lunch, cake and a few bubbles !
Thanks to funding from NHS Forth Valley endowment committee the event is free but you do need to book your space https://www.eventbrite.co.uk/e/talking-mats-is-21-tickets-62362171935
You can come to the morning only, afternoon only or come for the whole day.
If you can’t come to our event watch out for out blogs and social media celebrating the reach of Talking Mats for 21 days before the 15th of August .Please join in with your contributions using the hashtag #TMis21. For 21 days after our event we will be having a special Birthday offer! Watch this space, more to follow …….
Many thanks to Joan Murphy, our Talking Mats Founder, for this great blog sharing Jeppe Forchhammer’s thoughts about the importance of social communication – communicating ‘offline’ – for AAC users:
I met Jeppe Forchhammer at the 2019 ISAAC Conference in Denmark. We had an interesting conversation about the importance of social communication for AAC users and he kindly sent me this presentation and gave me permission to write a blog about his views.
Here are a few quotes from Jeppe but it is well worth reading his whole presentation
We have reached a time where communication systems become more and more electronic. I have noticed that children who need AAC ie augmented and alternative communication are starting more and more early. This I would like to question! In this lecture I will try to explain, why I think it is better to teach the children to use their body first. In order first to get direct communication relation to another person.
I think it is most important for an AAC user first to learn to interact with another person face to face. This is of course important for all infants in particular if they don’t have a spoken language. I think the eyes begins naturally to take over and the baby begin to communicate. At least I began to observe what happened around me using my eyes by watching things around me. In this way I began early to take contact with people around me.
I am afraid that AAC users in the future will lose some of their abilities to communicate with their body or facial expression. Especially if one starts too early. I think there is a risk that the child get blinkers and we have the risk that the child will be introvert. This might give the child some social problems if it doesn´t learn to use and read the body.
We must remember that a good relation is created face to face and not through a Speech Generating Device.
If they only communicate through their speech generating computer they may miss the face to face communication.
Many thanks to Jeppe for his thoughtful and stimulating comments.
If you would like to contact him, please email jeppeforchhammer@gmail.com
The importance of social and non-verbal communication is highlighted in our Talking Mats training courses. If you are interested in accessing this training take a look at our options here – https://www.talkingmats.com/training/